
In real-world settings outside of randomized trials, statin effectiveness for LDL-C lowering can be limited by medication nonadherence, statin-related symptoms, patient- or provider-concerns, and nocebo effects 2, 5, 6, 7, 8, 9, 10. For example, certain Asian groups may be at higher risk for statin-related side effects when prescribed high-intensity statins such as rosuvastatin 2. Recommendations may also be less certain in diverse racial/ethnic groups including heterogenous Hispanic or Asian populations. However, recommendations are less definitive for other groups such as patients with borderline or intermediate ASCVD risk, for whom decisions depend on individualized risk–benefit assessment. Thus, for patients with the highest ASCVD risk, guidelines recommend high-intensity statin therapy 2. High-intensity statins decrease LDL-C up to 50% in ideal, monitored clinical trial settings 4. For primary prevention, the 2018 American College of Cardiology (ACC)/American Heart Association (AHA) guidelines recommend estimating 10-year ASCVD risk using the Pooled Cohort Equations (PCE), a guideline-endorsed risk calculator, to guide statin therapy decisions. 
The primary goal of statin therapy is to adequately and sustainably decrease low density lipoprotein (LDL-C) levels and ASCVD risk 3. Cholesterol management through statin therapy is the cornerstone of ASCVD prevention 2. A data-driven personalized statin recommendation approach may inform shared decision making in areas of uncertainty, and highlight unexpected efficacy-effectiveness gaps.Ītherosclerotic cardiovascular disease (ASCVD) remains the leading cause of death in the United States 1. Recommendations included low- or moderate-intensity statins for maximum LDL-C lowering in nearly half the test set, which is discordant with their expected guideline-based efficacy. Overall, using aggregate EHR data, a personalized statin recommendation approach identified the statin intensity associated with the greatest LDL-C reduction in historical patients similar to a candidate patient. Among 8383 test-set patients, 52%, 44%, and 4% were recommended high-, moderate-, and low-intensity statins, respectively, for a maximum predicted average 1-yr LDL-C reduction of 16.9%, 20.4%, and 14.9%, in each group, respectively. 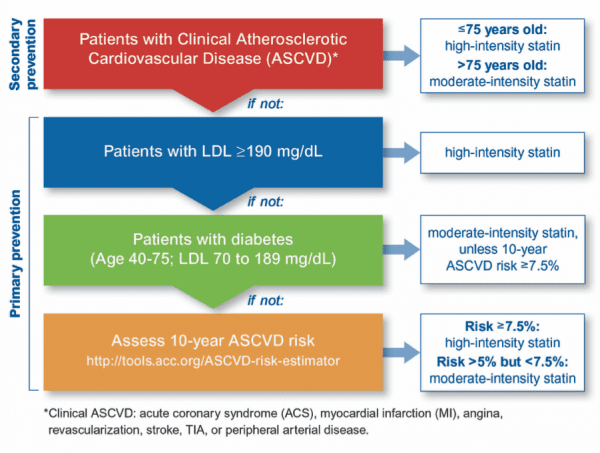
The overall cohort consisted of 50,576 patients (age 54.6 ± 9.8 years) with 55% female, 48% non-Hispanic White, 32% Asian, and 7.4% Hispanic patients. For each candidate patient, the algorithm recommended the statin decision that was associated with the greatest percentage reduction in LDL-C after 1 year in similar patients. 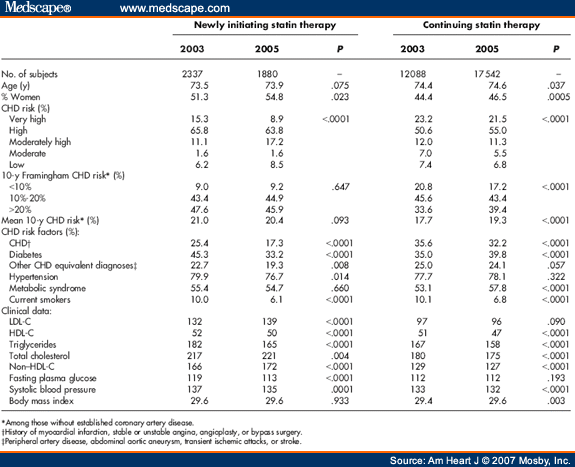
We modeled four statin decisions for each patient: none, low-intensity, moderate-intensity, and high-intensity. Weighted-K-nearest-neighbor (wKNN) regression models were used to identify historical EHR patients similar to a candidate patient. The cohort was split into training and test sets. Our retrospective cohort included adults from a large Northern California electronic health record (EHR) aged 40–79 years with no prior cardiovascular disease or statin use. We sought to develop a personalized statin recommendation approach for primary ASCVD prevention based on historical real-world outcomes in similar patients. In areas of clinical uncertainty, personalized approaches based on real-world data may help inform treatment decisions. Optimal statin therapy decisions rely on shared decision making and may be uncertain for a given patient. Statin therapy is the cornerstone of preventing atherosclerotic cardiovascular disease (ASCVD), primarily by reducing low density lipoprotein cholesterol (LDL-C) levels.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
